Borderline diabetes, also called prediabetes, affects millions of Americans, yet many people have no idea they have it. In fact, most people with prediabetes do not experience obvious symptoms at first.
That is what makes this condition so dangerous.
Your blood sugar levels may already be higher than normal, and your body may already be struggling with insulin resistance, long before you receive an official diagnosis. The changes often happen slowly over time, making them easy to overlook or blame on stress, aging, poor sleep, or a busy lifestyle.
The good news is that prediabetes is often reversible.
Recognizing the early warning signs gives you a chance to make changes before type 2 diabetes develops. Small improvements in your diet, activity level, weight, and daily habits can make a major difference in your long-term health.
In this guide, you will learn:
- What borderline diabetes actually means
- The most common symptoms to watch for
- Subtle warning signs many people miss
- Who is most at risk
- How doctors diagnose prediabetes
- What you can do to reverse it naturally
Key Takeaways
- Borderline diabetes means your blood sugar levels are higher than normal but not high enough for a diabetes diagnosis
- Many people with prediabetes have no noticeable symptoms
- Common warning signs include increased thirst, fatigue, frequent urination, and blurred vision
- Prediabetes can often be reversed through lifestyle changes
- Early action greatly reduces your risk of developing type 2 diabetes
- Simple changes in diet, exercise, sleep, and stress management can improve blood sugar control
What Is Borderline Diabetes?
Borderline diabetes is another name for prediabetes. It describes a condition where your blood sugar levels are elevated but not yet high enough to be classified as type 2 diabetes.
It is essentially a warning sign from your body.
At this stage, your body is beginning to struggle with insulin resistance. Diet plays a major role in improving insulin resistance and stabilizing blood sugar levels over time. Insulin is the hormone that helps move sugar from your bloodstream into your cells for energy. When your cells stop responding properly to insulin, sugar begins building up in your blood.
Over time, this can progress into type 2 diabetes if nothing changes.
The encouraging part is that prediabetes is often reversible, especially when caught early.
Common Symptoms of Borderline Diabetes
Many symptoms of prediabetes develop gradually. Because the changes happen slowly, people often ignore them or assume they are related to stress, aging, or lack of sleep.
Many of these warning signs overlap with other early blood sugar issues. You can also read our complete guide to prediabetes symptoms for a deeper breakdown of what to watch for.
Increased Thirst
Feeling thirsty all the time is one of the most common warning signs of elevated blood sugar.
When blood sugar levels rise, your kidneys work harder to remove the extra sugar from your bloodstream. This process pulls water from your body, which can leave you feeling constantly dehydrated.
You may notice:
- Dry mouth
- Constant thirst
- Needing to drink more water than usual
Frequent Urination
As your body tries to remove excess sugar through urine, bathroom trips become more frequent.
Many people notice this symptom most at night.
If you suddenly find yourself waking up repeatedly to urinate, especially along with increased thirst, it may be worth discussing with your doctor.
Fatigue and Low Energy
One of the most frustrating symptoms of borderline diabetes is persistent fatigue.
Even though there is sugar in your bloodstream, your cells may not be able to use it properly because of insulin resistance. As a result, your body struggles to produce energy efficiently.
You may feel:
- Tired after meals
- Drained throughout the day
- Weak during normal activities
- Exhausted despite getting enough sleep
Blurred Vision
High blood sugar levels can cause temporary swelling in the lenses of your eyes, which may lead to blurry or fluctuating vision.
Some people notice:
- Trouble focusing
- Vision changes that come and go
- Difficulty reading or seeing clearly
While occasional blurry vision can happen for many reasons, repeated vision changes should never be ignored.
Subtle Warning Signs Many People Miss
Some early symptoms of insulin resistance are less obvious but still important.
Increased Hunger and Sugar Cravings
If your cells are not receiving enough energy, your body may respond by increasing hunger signals.
You may feel hungry shortly after eating or experience strong cravings for sugary or carbohydrate-heavy foods.
This is not simply a lack of willpower. It can be a biological response to insulin resistance.
Slow-Healing Cuts and Bruises
Elevated blood sugar can interfere with circulation and immune system function, making it harder for your body to heal properly.
Small cuts, bruises, or scrapes may take much longer to heal than normal.
Tingling or Numbness in the Hands and Feet
Long-term elevated blood sugar can begin affecting nerves, especially in the extremities.
You may notice:
- Tingling sensations
- Burning feelings
- Pins-and-needles sensations
- Mild numbness in fingers or toes
These symptoms should not be ignored, especially if they happen repeatedly.
Darkened Skin Patches
Some people with insulin resistance develop dark, velvety patches of skin called acanthosis nigricans.
These patches commonly appear:
- Around the neck
- Under the arms
- In the groin area
- Around the knuckles
Skin tags may also appear in these areas.
These visible skin changes can sometimes be one of the earliest signs of insulin resistance.
Who Is Most at Risk for Prediabetes?
Certain risk factors increase the likelihood of developing borderline diabetes.
Age
Risk increases after age 45, although younger adults and even children can also develop prediabetes.
Family History
If you have a parent or sibling with type 2 diabetes, your risk is significantly higher.
Excess Weight
Being overweight, especially carrying excess abdominal fat, strongly increases insulin resistance. Understanding how age and obesity affect diabetes risk can help you better recognize the factors that contribute to insulin resistance and prediabetes.
Physical Inactivity
Regular movement helps your body use insulin more effectively. A sedentary lifestyle increases your risk.
Certain Medical Conditions
Your risk may also increase if you have:
- High blood pressure
- High cholesterol
- Polycystic ovary syndrome (PCOS)
- A history of gestational diabetes
Ethnic Background
Prediabetes is more common among:
- African Americans
- Hispanic and Latino Americans
- Native Americans
- Pacific Islanders
- Some Asian American populations
Why Early Detection Matters
Prediabetes often develops silently.
Even if you feel fine, elevated blood sugar may already be affecting your blood vessels, nerves, heart, kidneys, and metabolism.
Catching it early gives you the best chance to reverse the condition naturally.
Research shows that losing just 5% to 10% of your body weight can significantly improve blood sugar control and lower your risk of developing type 2 diabetes.
For many people, relatively small lifestyle changes lead to major health improvements.
How Doctors Diagnose Borderline Diabetes
Prediabetes is usually diagnosed through a simple blood test. In many cases, people discover they have borderline diabetes during a routine checkup before noticeable symptoms appear.
Doctors commonly use one or more of the following tests:
A1C Test
The A1C test measures your average blood sugar levels over the past two to three months.
An A1C between 5.7% and 6.4% typically indicates prediabetes.
Fasting Blood Sugar Test
This test measures your blood sugar after fasting overnight.
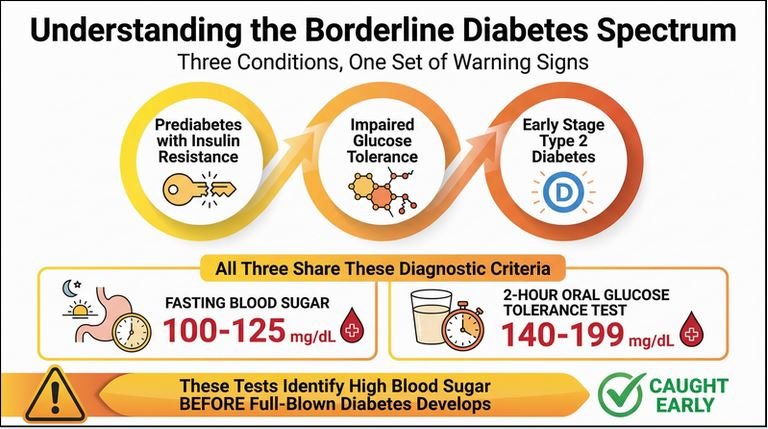
A fasting blood sugar level between 100 and 125 mg/dL is considered prediabetes.
Oral Glucose Tolerance Test
This test checks how your body responds to sugar after drinking a glucose solution.
A blood sugar level between 140 and 199 mg/dL after two hours may indicate prediabetes.
Blood Sugar Levels That Indicate Prediabetes
Doctors typically use three different tests to diagnose prediabetes.
You may be diagnosed with prediabetes if your results fall within these ranges:
- A1C between 5.7% and 6.4%
- Fasting blood sugar between 100 and 125 mg/dL
- Oral glucose tolerance test between 140 and 199 mg/dL after two hours
If you are unsure what your blood sugar numbers mean, our blood sugar chart can help you better understand healthy and elevated glucose ranges.
These numbers indicate that your body is having trouble regulating blood sugar effectively.
What This Means for You
Getting tested can feel intimidating, especially if you are worried about the results. But early testing gives you the best opportunity to make changes before type 2 diabetes develops.
For many people, identifying prediabetes early becomes the turning point that leads to healthier habits and better long-term health.
When You Should See Your Doctor
You should talk to your doctor if:
- You notice symptoms of elevated blood sugar
- You have multiple risk factors
- You are over age 35 and have not been screened recently
- You have a family history of diabetes
- You are overweight or inactive
Seek medical attention sooner if you experience:
- Extreme thirst
- Rapid unexplained weight loss
- Severe fatigue
- Sudden vision changes
Early testing can help prevent years of unnoticed damage.
Possible Complications of Untreated Prediabetes
Prediabetes does not always progress to type 2 diabetes, especially when caught early. However, consistently elevated blood sugar can begin affecting your body long before a diabetes diagnosis happens.
Over time, untreated prediabetes may increase the risk of:
- Type 2 diabetes
- Heart disease
- Stroke
- Nerve damage
- Kidney problems
- Vision changes
The important thing to remember is that these complications are not inevitable.
Early lifestyle changes can significantly reduce your risk and help protect your long-term health. Even small improvements in diet, activity level, weight, and sleep can make a meaningful difference over time.
How to Reverse Borderline Diabetes Naturally
For many people, prediabetes can be improved or even reversed through lifestyle changes.
The goal is not perfection. The goal is consistent progress.
Focus on Balanced Meals
Building balanced meals can help stabilize blood sugar levels.
Try to include:
- Non-starchy vegetables
- Lean protein
- Healthy fats
- High-fiber carbohydrates
Good choices include:
- Leafy greens
- Broccoli
- Salmon
- Chicken
- Beans
- Oatmeal
- Brown rice
- Berries
Limiting sugary drinks and heavily processed foods can also make a major difference.
Certain foods may help support more stable blood sugar levels naturally. Our guide to foods that lower blood sugar explains which foods may be most helpful.
Some people also benefit from following a low glycemic diet focused on foods that cause slower blood sugar rises.
Increase Physical Activity
Exercise improves insulin sensitivity and helps your body use glucose more effectively.
Aim for about 150 minutes of moderate activity per week.
Helpful activities include:
- Walking
- Swimming
- Cycling
- Dancing
- Strength training
Even short walks after meals can help lower blood sugar.
Aim for Gradual Weight Loss
Losing even a small amount of weight can improve insulin resistance significantly.
You do not need extreme diets or rapid weight loss programs to see benefits.
Slow, steady progress is usually more sustainable.
Improve Sleep and Stress Management
Poor sleep and chronic stress can both raise blood sugar levels.
Helpful strategies include:
- Maintaining a regular sleep schedule
- Practicing deep breathing
- Taking short walks
- Spending time outdoors
- Limiting screen time before bed
- Making time for relaxing activities
What This Means for You
You do not need to make perfect changes to improve your health.
Small, consistent habits like walking more, improving meals, and getting better sleep can meaningfully improve blood sugar levels over time.
Frequently Asked Questions
Can borderline diabetes be reversed?
Yes. Many people can reverse prediabetes through weight loss, healthier eating, exercise, and lifestyle changes.
Do all people with prediabetes develop type 2 diabetes?
No. Prediabetes does not always progress to diabetes, especially when caught early and treated appropriately.
Can you have prediabetes without symptoms?
Yes. Many people have no noticeable symptoms at all. This is why routine screening is important.
Final Thoughts
Borderline diabetes is common, but it does not have to become permanent.
Your body often gives warning signs long before type 2 diabetes develops. Recognizing those signs early gives you an opportunity to take control of your health while there is still time to reverse course.
You do not need to make perfect choices every day to improve your health.
Small, steady improvements in your diet, activity level, sleep, and daily habits can significantly reduce your risk and help restore healthier blood sugar levels over time.
If you think you may have symptoms of prediabetes, talk with your doctor about getting tested. Early action can make a tremendous difference in your future health.
